Flexible Sigmoidoscopy
What is a flexible sigmoidoscopy?
It is an examination, which allows the endoscopist to look directly at the lining of the lower part of your bowel. See the diagram. This is done using a sigmoidoscope (a flexible tube about the thickness of an index finger). Sometimes a sample of the lining of the bowel (biopsy) is taken for laboratory examination. If polyps are found, they can be removed during the examination.
Preparation for the test
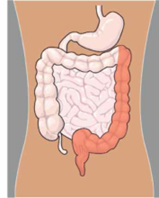 | For this examination to be successful and allow a clear view of the colon, your bowel must be as empty as possible. If the bowel is not sufficiently empty the whole procedure may have to be cancelled and repeated on another occasion. This is due to the high possibility of the endoscopist missing important signs. (It is believed that those patients who have a bowel cancer diagnosed within two years of a previous colonic examination have probably had it missed at the time of the original examination - this scenario is now labelled Post Colonoscopy Colorectal Cancer Syndrome PCCCS). As part of your preparation you will be given a laxative. It is important to follow the advice given about bowel preparation. |
- If you have diabetes or haemophilia, please discuss with your consultant or pre assessment nurse one week before your test.
- If you are taking warfarin, clopidogrel, or other blood thinning medications, please inform us at least one week before the test.
- If you have a pacemaker or ICD, please inform us at least one week before the test.
- You may continue to take other medications as normal, except iron tablets or stool bulking agents (such as Fybogel, Regulan, Proctoibe) which should be stopped one week before your examination.
- Please bring a list of any medications you are currently taking. If you have any queries about your medication please ring the ward.
- It is especially important to remember to bring any asthma inhalers or angina sprays with you.
- Do not bring any valuables to the ward.
- Please remove your nail polish and all types of false nails before attending for your procedure.
- Please bring with you your dressing gown, slippers, and something to read during your stay.
- Patients feel a spare set of underwear is useful.
Click the link for a Flexible Sigmoidoscopy Timetable and Diet Sheet
FAQs
This test is very safe, but there are some risks associated with this procedure.
These include:
- A reaction to the sedative. The sedative can affect your breathing making it slower and more shallow;
- When a biopsy is taken or a polyp is removed, there may be a little bleeding but this is rare. (Risk approximately one for every 100 to 200 examinations where a polyp is removed). If this does not stop within 24 hours or is excessive, please contact the Spencer Private Hospital Ward or Accident and Emergency (A&E);
- Perforation, which is a little tear in the wall of the colon, this is also rare. (Risk approximately one for every 1000 examinations). This would require a short stay in hospital and treatment with antibiotics, or very occasionally may require surgical repair;
- A feeling of bloating due the air insert to enable the consultant to see clearly.
Please talk to your endoscopist before your examination if you have any worries about these risks.
Yes, there is a CT Pneumocolon and a Barium Enema. They both require the same kind of bowel preparation as a colonoscopy, but they do not allow the removal of polyps or the taking of biopsies.
This means that you would probably require a flexible sigmoidoscopy anyway.
- Your throat may be sprayed with a local anaesthetic that has a numbing affect; this has a slightly bitter taste.
- You will be asked to lie on your left side with your left arm behind your back as you may be turned onto your stomach during the test.
- Then while you are lying on your left side, a small mouth-guard will be placed in your mouth in order to protect your teeth.
- A sedative and painkiller are given before the examination. This will help you feel more relaxed and sleepy. (This needle will be left lightly strapped to your hand/arm until you are recovered from the procedure for any other drugs that may be needed).
- A small device for recording the pulse and breathing will be attached to your finger and you will be given oxygen
- A cuff will be placed on your arm to monitor your blood pressure if you have sedation (please inform the nurse if there is a reason why a certain arm cannot be used).
- Three small dots will be placed on your back to monitor your heart during the procedure.
- A sticky pad may be placed on your thigh if diathermy is needed during the procedure
- Once you are sleepy the endoscopist will begin the test.
- The stomach and duodenum will be gently inflated with air to expand it so the lining can be seen more clearly. The air is sucked out at the end of the test.
- A muscle relaxant is given to stop your bowel moving.
- The nurse may need to clear saliva from your mouth using a small suction tube.
- If a narrowing is found in the bile duct, a small plastic tube (stent) is inserted to allow the bile to drain. This may stay in place permanently or be removed at a later date.
- If the endoscopist finds a gallstone(s) in the bile duct during the ERCP, the opening of the bile duct will be enlarged with a cut using an electrical current (diathermy). This will allow the stones to be removed. If the stone is very large, or if there are a lot of stones, it may not be possible to remove the stone(s) in one go. In this case a stent is left in the bile duct and a further appointment will be arranged.
- A biopsy (a small sample of the lining of your bowel) may be taken during the examination to be sent to the laboratory for more tests. You cannot feel this. (A video recording and/or photographs may be taken for your records). Afterwards the duodenoscope is removed easily.
- In about one in 20 cases it will not be possible to treat your problem at ERCP. For example, the opening of the bile duct may be too narrow to allow the catheter to be inserted. If this occurs, then further treatment options will be discussed with you after the test.
- Please report to the reception of Spencer Private Hospital.
- You will then be taken to the ward.
- A nurse will check your details, blood pressure, and pulse. If you are allergic to anything (such as medicine, latex, plasters), please tell the nurse.
- Please do not hesitate to ask any questions you may have.
- You will have the test explained to you during your admission. You will then be asked to sign a consent form.
- You will need to remove all your clothes and put on a hospital gown and dignity shorts.
- You will be asked to remove any spectacles, contact lenses, tongue studs, and dentures (if you have them).
- A nurse will stay with you throughout the examination.
- You will return to the ward area to rest.
- Once recovered you may eat and drink as normal.
- You may still have a little wind; this is natural.
- The nurse will tell you the result of the examination before you go home. Any biopsy result will take longer.
- After sedation, you may feel a little lightheaded for the remainder of the day.
- A letter will be sent to your GP.
- If you had the sedative injection you must have a friend or relative with transport to collect you from the ward and stay with you at home for at least 24 hours until you are fully recovered
- You are advised not drive, drink alcohol, operate machinery (including an electric kettle), or sign important documents for 24 hours following the sedative;
- You may notice that your bowels do not return to normal for a few days following the procedure.
